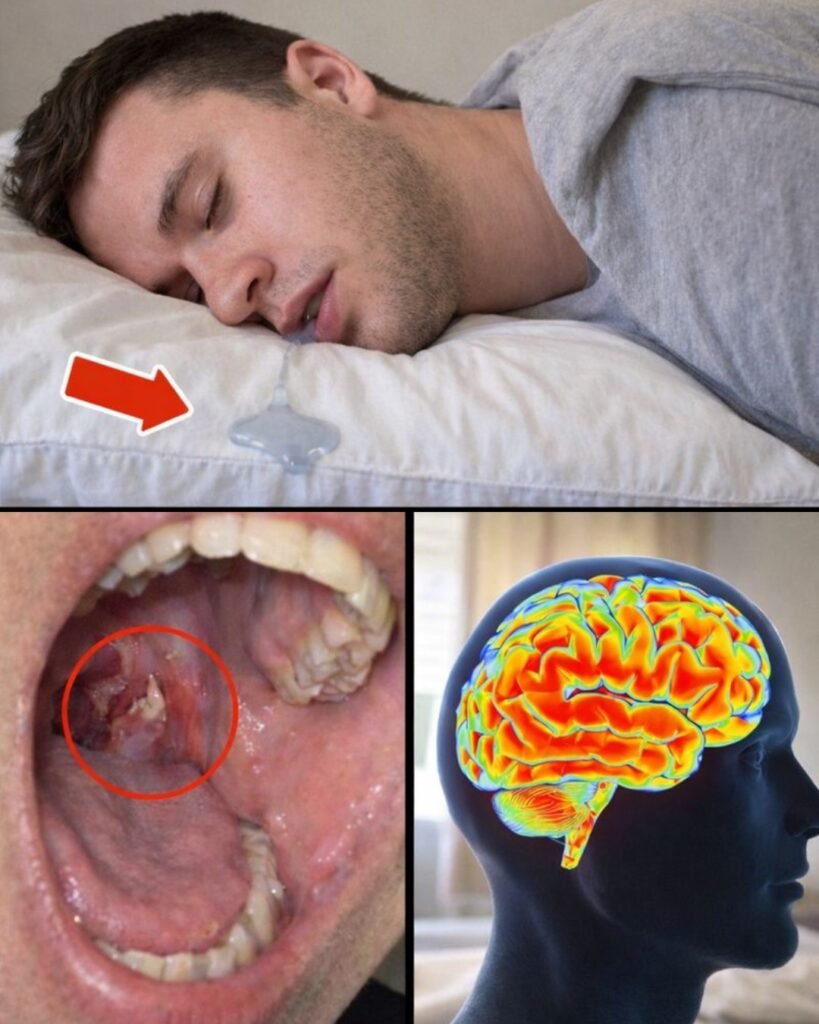
Waking up to a wet pillow and dried saliva at the corner of your mouth can leave you feeling embarrassed and a bit unsettled. You might brush it off as just a quirky sleep habit, but when it happens night after night, that damp spot becomes a nagging reminder that something might be off. Excessive drooling during sleep—medically known as nocturnal sialorrhea—often stems from relaxed muscles, mouth breathing, or slowed swallowing while you rest. Research from sources like the Cleveland Clinic and Sleep Foundation shows it’s surprisingly common in adults, yet many ignore it until it pairs with other bothersome signs like snoring, fatigue, or heartburn.
The good news? Understanding the potential underlying causes can lead to simple changes or professional guidance that brings real relief. But here’s the part most people overlook: what seems like a minor annoyance could be your body’s quiet way of flagging something worth checking. Stick with me as we uncover the eight most common conditions linked to nighttime drooling—and why getting ahead of them might transform your mornings.

Why Drooling Tends to Happen More at Night
During the day, you swallow frequently—up to once per minute—keeping saliva under control. At night, things change. Saliva production continues (though at a lower rate), but swallowing reflexes slow dramatically, and facial muscles relax deeply. Gravity pulls saliva toward the corners of your mouth, especially if you’re sleeping on your side or stomach.
Add in mouth breathing from nasal issues or other factors, and drool escapes more easily. Studies highlight that conditions affecting breathing, swallowing, muscle control, or saliva production amplify this effect. While occasional drooling is harmless, persistent cases often tie back to treatable issues.
But that’s not the full picture. Let’s look at the top conditions experts from places like the Mayo Clinic, Cleveland Clinic, and Sleep Foundation frequently connect to nighttime drooling.
The 8 Conditions Commonly Linked to Nighttime Drooling
Here are the most reported links in adults, drawn from trusted medical sources.
8. Nasal Congestion or Sinus Issues
Stuffy nasal passages from allergies, colds, or chronic sinusitis force mouth breathing. With your mouth open, saliva slips out more readily during deep sleep phases.
This is often temporary, but recurring congestion can make drooling a nightly issue. Many notice it worsens during allergy seasons.

7. Gastroesophageal Reflux Disease (GERD)
Acid reflux irritates the esophagus and throat, prompting extra saliva production as a protective response. Lying flat worsens reflux, leading to more saliva pooling overnight.
Research links GERD to increased nocturnal sialorrhea, sometimes with a sour taste or choking sensation upon waking.
6. Medication Side Effects
Certain medications stimulate salivary glands or alter muscle control, causing hypersalivation. Common culprits include some antipsychotics, Alzheimer’s drugs, or cholinergic agents.
If drooling started after a new prescription, this reversible factor often ranks high on doctors’ lists.
5. Obstructive Sleep Apnea (OSA)
In OSA, airway collapses cause breathing pauses, leading to mouth breathing and relaxed throat muscles. This setup allows excess saliva to escape.
Studies show a strong association between sleep apnea, snoring, daytime fatigue, and nighttime drooling.
4. Infections or Throat Irritation
Swollen tonsils, post-nasal drip, or throat infections increase mucus and saliva while making swallowing harder. Viral or bacterial causes can temporarily overwhelm normal control.
Persistent irritation signals the need for further evaluation.

3. Stroke or Recent Neurological Event
A stroke can cause one-sided facial weakness, impairing lip closure or swallowing. Drooling may appear suddenly post-event.
Experts stress prompt medical attention for new-onset cases, especially with speech changes or weakness.
2. Parkinson’s Disease
Parkinson’s often reduces coordinated swallowing, allowing saliva to pool. Up to 80% of patients experience sialorrhea, sometimes as an early sign alongside tremors or stiffness.
It’s tied to slowed muscle movements rather than excess production.
1. Other Neurological Conditions
Disorders like multiple sclerosis, ALS, cerebral palsy, or similar issues disrupt nerve signals to swallowing muscles. This leads to chronic poor saliva management.
Progressive conditions make this a frequent concern.
Here’s a quick comparison table of these conditions and their key clues:
- Sleep Apnea & Nasal Congestion → Mouth breathing → Snoring, daytime fatigue, frequent waking
- GERD & Infections → Excess saliva or mucus → Heartburn, sore throat, post-nasal drip
- Medications & Stroke → Impaired control → Recent med changes, sudden onset, speech issues
- Parkinson’s & Neurological Issues → Muscle/nerve dysfunction → Tremors, stiffness, progressive symptoms

Real-Life Examples: When People Took Action
Consider someone like Laura, in her late 50s, who dealt with worsening drooling and loud snoring. A sleep study confirmed obstructive sleep apnea; starting CPAP therapy dramatically cut the drooling and boosted her energy levels.
Or David, 65, who linked his wet pillows to frequent heartburn episodes. Simple GERD management—diet tweaks and elevating his head—brought noticeable improvement in his sleep quality.
These stories highlight how recognizing patterns and seeking help often leads to meaningful change.
Practical Steps You Can Take Right Now
Occasional drooling is normal, but if it’s frequent or disruptive, start with these safe, at-home approaches:
- Track it: Keep a simple sleep diary noting frequency, sleep position, and any related symptoms (snoring, heartburn, congestion).
- Adjust position: Try sleeping on your back with a supportive pillow to let gravity help keep saliva in place.
- Ease congestion: Use saline nasal sprays, a humidifier, or over-the-counter decongestants (if suitable for you) to promote nasal breathing.
- Review habits: Elevate your head slightly for reflux, stay hydrated, and discuss medications with your doctor if timing aligns.
- Monitor closely: Note if symptoms like fatigue, choking sensations, or neurological changes appear.
These tweaks help many without needing more intervention.
When Should You See a Doctor?
Seek professional advice if drooling:
- Happens nightly and affects sleep or confidence
- Comes with snoring, excessive tiredness, or breathing pauses
- Appears suddenly or with weakness, speech changes, or tremors
- Pairs with heartburn, persistent congestion, or medication starts
A primary care doctor, ENT specialist, or sleep expert can guide evaluations like exams or studies.
FAQ
Is drooling while sleeping always a problem?
No—many people experience it occasionally due to sleep position or temporary congestion. It’s usually harmless unless persistent or accompanied by other symptoms.
Can changing my pillow or mattress help stop drooling?
Possibly. A firmer pillow that supports back sleeping or keeps your head elevated can reduce mouth opening and saliva escape for some.
Does stress or anxiety contribute to nighttime drooling?
It can indirectly—stress may worsen conditions like bruxism (teeth grinding) or mouth breathing, increasing saliva flow or relaxation issues.
Waking up to dry pillows and feeling refreshed is possible for most. These eight conditions offer clear starting points to explore why it happens and how to address it. A simple conversation with your healthcare provider could uncover the key to better nights.
This article is for informational purposes only and is not a substitute for professional medical advice. Always consult your healthcare provider for personalized guidance regarding any health concerns.